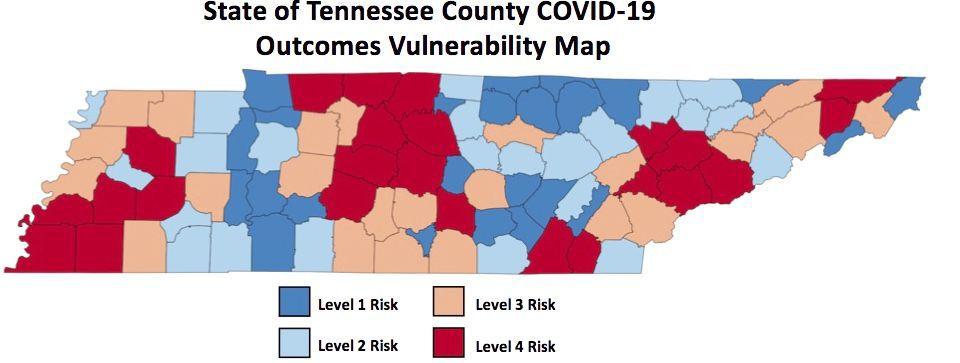
Model: County At Risk In Second Wave Of Virus

Featured on the GreenevilleSun.com, read the full article here.
Greene County is one of the Tennessee counties at risk for poor patient outcomes if a second wave of the coronavirus occurs according to predictive analytics by a Nashville healthcare tech company.
Rural counties near major population centers, like Greene, could see a second wave of COVID-19 in the summer or fall according to the predictive model developed by Decode Health, a health management analytics company.
Decode Health’s model does not predict the number of cases for a county, but at what risk the community is for poor patient outcomes such as hospitalization and/or deaths.
In the latest model released this week by the company, Greene County is at a “Risk 3” level for hospitalizations and/or deaths in a second wave of the virus. In its first model released the week of May 5, Greene County was defined as a “Risk 4,” the level with the highest possibility of poor outcomes.
Ballad Health is continuously studying its models about what could occur in the future with the coronavirus in the region to provide direction in regard to a second wave, Dr. Clay Runnels, chief physician executive for the system, said Friday.
While Ballad Health was not involved with the Decode Health analytics, Runnels said the model points to why people should continue to following recommended precautions to limit the spread of the virus.
“Its prediction is something that every health official fears — a second wave of cases concentrated in our more rural counties,” Runnel said.
One of the things to remember about models is that while they are important for planning, they are not an indication that something will definitely happen, which is why health officials continue to stress the practice of precautions, he said.
“It is still very important to practice social distancing,” he said. “It is still very important to avoid large gatherings and to wear facial coverings in enclosed public spaces. These are the things everyone needs to do to avoid a rise of cases in our region.”
“Certainly, if we don’t do that, what they are predicting could be a reality,” Runnels continued.
While the number of new cases has flattened regionally, the results of the reopening may not be reflected in virus case numbers for a few weeks as people may not show symptoms for some time after being infected and the time needed for testing, he said.
MODEL DEVELOPMENT
Data is key in making decisions about how to proceed in further reopening the economy and the planning of efforts to limit a possible second wave of the virus, according to Decode Health CEO and founder Chase Spurlock.
By sharing its predictive models with community leaders and governments, Decode Health hopes that the information can be used to address a second wave before it happens.
“We need to actively use data if we want to be proactive in addressing a second wave of the virus,” he said. “If we wait to be reactive after a second wave occurs, it will lead to a bad situation. It will be too late.”
Decode Health uses artificial intelligence models to predict and monitor chronic diseases such as multiple sclerosis, Crohn’s disease and kidney disease. Spurlock explained that a deep knowledge of the disease is coupled with expert data modeling techniques to help identify patients who may be heading toward a diagnosis or serious health episode earlier than conventional approaches.
When the COVID-19 pandemic began, the company decided to use its expertise to develop a predictive model for the virus with three goals in mind on how to use the data — spotlight counties where infections are likely to emerge, define characteristics for counties where the worst outcomes including death are likely to occur, and monitor infection rates to understand positive or negative trends weeks in advance.
The analytical model integrates data about the number of cases, hospitalization and demographic information available from the State of Tennessee and other sources such as John Hopkins University and the New York Times.
“We use this data and our own propriety analytics that allow us to look at social, physical and environmental factors that contribute to disease emergence,” Spurlock said.
These factors include a prevalence of health conditions such as diabetes, access to quality health care facilities inside a county, the level of food insecurity and socio-economic status.
The models continue to evolve as more data becomes available, he said, but some trends are emerging.
One is that rural counties near major population centers are likely to be where the second wave of the disease emerges, Spurlock said. And due to travel between these counties and nearby large cities for such reasons as work, medical care, entertainment and shopping, the virus could then re-emerge in greater numbers in those communities as well.
In the May 11 model, both Washington and Sullivan counties are designated in the highest risk level. Neighboring counties such as Greene, Hawkins, Carter and Hamblen counties are designated in the next highest risk level.
Spurlock said that people should pay attention to what is happening in relation to the coronavirus in neighboring counties, which will help them avoid communities with higher case numbers.
FOCUSED EFFORT
Julia Polk, a co-founder of Decode Health, said that as more robust data becomes available about the coronavirus, it can help identify trends and better inform decisions about how to direct efforts to lessen the impact of the illness.
For example, one trend identified both in the state and nationwide is the higher risk that African-Americans have from experiencing severe COVID-19 complications, Polk said.
Recent data has also shown a rise in serious complications in the Hispanic and Asian-American communities, she said, which could direct more focused research into why it is occurring and how those trends can be reversed
The information available about the virus and its breakdown also continues to change. Although it is not yet publicly available, the state is reported to have begun compiling data on a zip code level, Polk said.
Once that data is available, it could be used to refine what areas are reopened and how based on the prevalence of the virus in sections of a community, she said.
Zipcode information could also be used to plan educational campaigns or testing efforts in neighborhoods where the numbers of virus cases are higher, Polk continued.






